What does it take to fight cancer when the nearest cancer hospital is 8-hours away?
Before the establishment of Binaytara Foundation Cancer Center in Janakpurdham, Nepal in December 2018, for cancer patients in Nepal’s Madhesh Province, fighting cancer meant traveling 8-hours by bus to the nearest cancer hospital where most providers do not speak your language.
For them, it meant leaving their loved ones behind to fight cancer alone, in a place where they might not speak the local language, might not understand the culture, and might not know what is going on with their health.
Finally a Cancer Hospital for more than 6 million People of Madhesh Province
December 2018
Binaytara Foundation Cancer Center (BTFCC) rents a building in Janakpurdham, and starts providing oncology services to people of Madhesh Province.
February 2019
A weekly virtual tumor board with experts in the US is started to help with the management of cancer patients at BTFCC.
August 2020
BTFCC trains female community health volunteers to improve awareness about cervical caner screening. A city-wide cervical cancer screening program is started in Janakpurdham.
December 2021
BTFCC purchases land in Janakpurdham, Nepal to build a 200-bed state of the art cancer hospital that will serve as the center of excellence for research, education, and patient care.
February 2022
Binaytara Foundation Cancer Center (BTFCC) becomes all paperless hospital with the implementation of electronic Health Record system and Human Resource Management system.
March 2022
Ground-breaking ceremony is held for the construction of a 200-bed cancer hospital in Janakpurdham, Nepal.
March 2022
Head & Neck Surgery & Histopathology departments are established at the Binaytara Foundation Cancer Center.

About The Binaytara Foundation Cancer Center
The Binaytara Foundation Cancer Center is a cancer hospital in Janakpurdham, a city in southeast Nepal. It was established by the Binaytara Foundation in 2018 to meet the cancer care needs of more than six million residents of Madhesh Province (then province 2) who were forced to travel more than 8-hours by bus for cancer care at the nearest cancer hospital.
Current Services
The Binaytara Foundation Cancer Center currently provides cancer prevention, diagnosis, treatment, and palliative care services.
The following list of services are among the growing list of healthcare services the BTFCC offers:
- Chemotherapy
- Head & Neck Surgery
- 24-hour emergency services
- 24-hour in-patient care
- Histopathology & other lab services
- Other Surgical Services
- Cancer Screening
- 24-hour ICU care
- Gynecological oncology
BINAYTARA FOUNDATION CANCER CENTER, NEPAL
Cutting Edge, Evidence-Based, Culturally-Appropriate Cancer Care for the People of Nepal & India
Imagine you are living in a place where there are no trained oncology care providers, no healthcare facilities to diagnose cancer, and no information source to educate you on cancer prevention. Then you start feeling sick and visit a drug store (the first point of contact for all healthcare needs for millions of people living in low-income countries) to get advice and medicine for your symptoms.
You buy the medicine from the drugstore, go home and take medicine exactly as advised by the drugstore clerk (most likely a layperson with no healthcare training). You feel as if the symptoms were relieved for a few days, but they came back. You go to the same drugstore or to a different one this time. You take a different medicine this time based on the drugstore clerk's advice or you may see a doctor at the drugstore. The symptoms persist or get worse. You try to ignore them and keep going with life, but it worsens daily.
Then someone tells you to go to the big city for treatment. You and your fourteen-year-old son take an early morning bus and reach the city in the evening. You spend the night at a lodge near the doctor's office. The following day you visit the doctor's office. After waiting for a few hours, it is your turn to be seen. The doctor asks a few questions in a language you don't fully understand. You try to explain your symptoms, but the doctor doesn't understand your language and asks your son (who speaks the language) to explain. You just nod your head and look at your son as he tries to explain your symptoms to the doctor. The doctor scribbles something on the paper and asks you to buy some medicines and get some tests.
You and your son spend the next few days/weeks in the city getting all the tests done. After a few weeks, the results are back, the doctor explains everything to your fourteen-year-old son, and you just nod your head. Your son starts crying; you ask him to tell you everything the doctor said to him, but he just cries. Then you hear the word "cancer."
You don't know anyone who has survived cancer. In your home state, there is no cancer doctor, no cancer care facility, and no awareness and education about cancer. The only thing you know about cancer is that you die when you get cancer.
The above story is a real-life experience of Rupesh Lal, a 45-year old man from a town in Southeast Nepal. Until February 2016, Rupesh was a very healthy man who ran his convenience store in the heart of the city and had respectable earnings. He sent both of his sons to a nearby private school and was an active member of his community. When Rupesh was diagnosed with a type of blood cancer, his world fell apart.
Even though Rupesh could afford to get treatment in the city, it was not convenient. He could not speak the language, he had no family around, he missed the local ethnic food, and his son missed months of school. The family back home constantly worried because they could not be with him when he was going through the rough side effects of the cancer treatment and the complications of the procedures he underwent.
He decided to return home against his doctors’ advice, and he came back before finishing his treatment. Though Rupesh did not beat cancer, he received palliative care services from clinicians trained by the Binaytara Foundation as part of our hospice & palliative care training programs in Nepal.
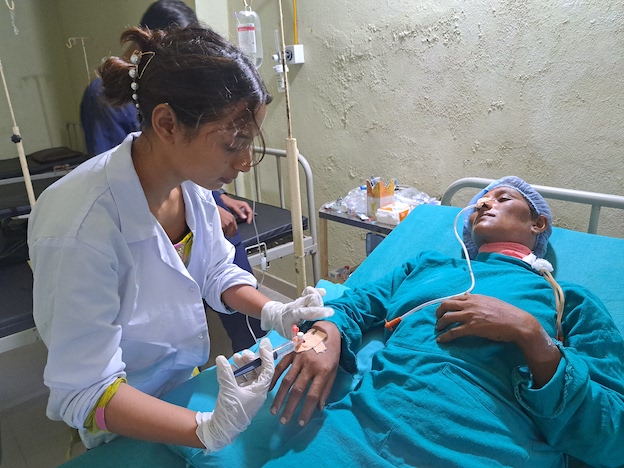
In December 2018, we opened a 25-bed cancer hospital – Binaytara Foundation Cancer Center (BTFCC), in Janakpur, Nepal. BTFCC is the first and only cancer hospital in Madhesh Province, a state with more than six million people. Today, BTFCC offers state-of-the-art cancer prevention, early detection, cancer treatment, chemotherapy, surgical oncology, palliative care, ICU, in-patient care, and laboratory services. The pharmacy supplies services to cancer patients and non-cancer patients in the region. The hospital employs several dozen healthcare providers, including oncologists, surgeons, medical officers, nurses, and laboratory staff.
Every Sunday, doctors at BTFCC present patient cases to a virtual Tumor Board of 10 to 15 international physicians. The video consultations include surgeons, oncologists, and pathologists who donate their time to review patient cases. This helps doctors at the hospital to broaden their knowledge and explore treatment options. Other physicians from Nepal and India also take part to improve their knowledge of cancer care.
Under the best circumstances, individuals seeking cancer care in the region around Janakpur, Nepal, have had to travel eight hours to the nearest cancer center in the capital city of Kathmandu or Bharatpur, Chitwan. Most cannot make the trip due to a lack of transportation, poor road conditions, work obligations, and even a local language barrier. Unfortunately, patients with cancer are often undiagnosed or diagnosed at terminal stages. A local cancer care hospital where the disease can be detected and treated early is essential to save lives. As such, BTF founders and the board believe it is time to respond to this critical need in Nepal by building a cancer hospital.
Email Newsletter Signup
We Advocate, Educate and Innovate to Improve Access to Cancer Care
